The Repeat ECG Problem: How Serial Placement Inconsistency Is Bleeding Your Hospital of Time, Money, and Diagnostic Credibility
Over 300 million ECGs are performed worldwide each year, with more than 100 million in the United States alone. The ECG is the most commonly performed cardiovascular diagnostic procedure in medicine. But here is the problem that rarely appears on any hospital's balance sheet: a significant percentage of those ECGs are compromised at the point of acquisition because the electrodes were placed incorrectly.
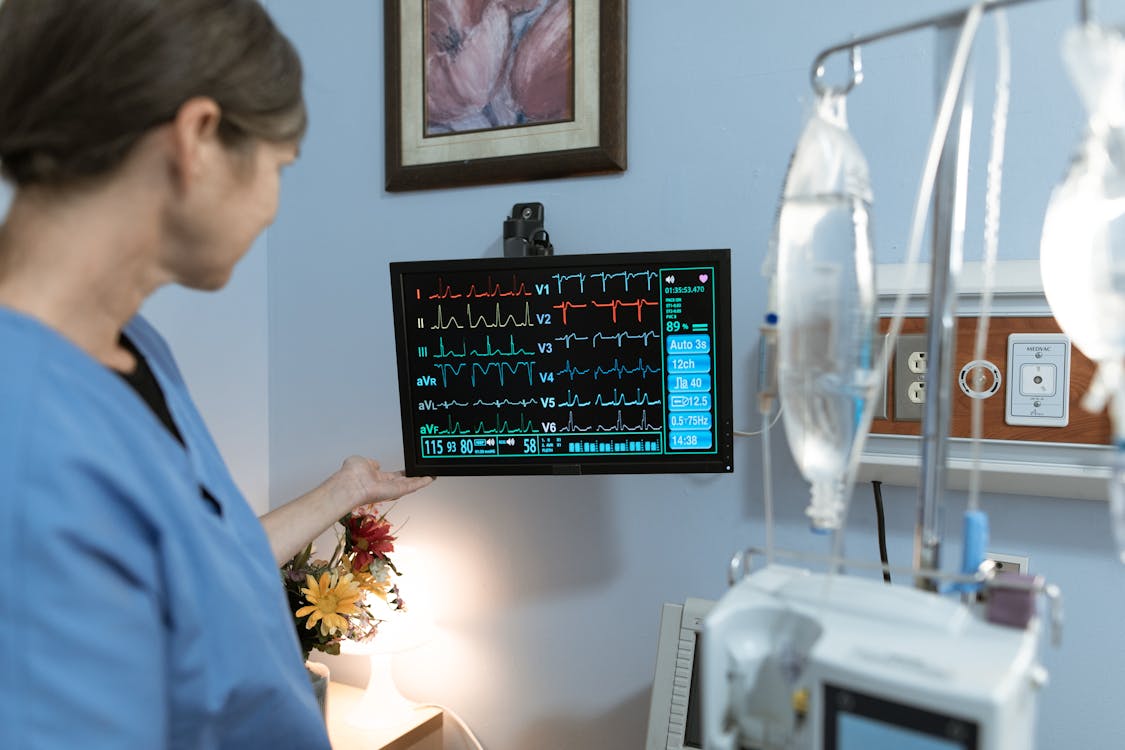
A Financial and Operational Analysis for Hospital Leadership
EXECUTIVE SUMMARY: Electrode misplacement on serial ECGs creates diagnostic confusion that triggers unnecessary downstream testing, delays treatment, extends length of stay, and exposes hospitals to malpractice liability. A peer-reviewed Cureus study estimates the cost of ECG lead mispositioning to CMS alone at $3.2 billion annually. This brief explains why it happens, what it costs your institution, and what technology exists to eliminate it.
The Business Case: Why Your CFO Should Care About Electrode Placement
Over 300 million ECGs are performed worldwide each year, with more than 100 million in the United States alone (GE HealthCare; Circulation: Cardiovascular Quality and Outcomes). The ECG is the most commonly performed cardiovascular diagnostic procedure in medicine. At a Medicare reimbursement rate of $16.46 per ECG ($8.30 facility fee, $8.16 professional fee), the annual U.S. expenditure on computerized ECGs exceeds $2 billion (ScienceDirect, 2020).
But here is the problem that rarely appears on any hospital’s balance sheet: a significant percentage of those ECGs are compromised at the point of acquisition because the electrodes were placed incorrectly. And when a compromised ECG is compared to a subsequent ECG acquired with different electrode placement, the resulting discrepancies trigger a cascade of costly clinical decisions.
$3.2B
Estimated annual cost to CMS from ECG lead mispositioning alone — driven by downstream testing triggered by false patterns like poor R-wave progression. (Rehman et al., Cureus, 2020)
50%+
of all ECGs have at least one significant electrode placement error, most commonly V1 and V2 placed too high. (Multiple studies cited in Circulation; GE HealthCare; JEMS, 2025)
45%
of serial ECGs have inconsistent electrode placement — meaning clinicians are comparing tracings that were acquired from different anatomical positions. (Med-Linket clinical analysis)
10.8%
of ECGs in one study were found to have patterns possibly falsely labeled as myocardial infarction due to suspected precordial lead mispositioning. (Rehman et al., Cureus, 2020)
5%
of all ECGs are performed with a lead reversal, per the ACC and AHA. (Hillrom/Baxter, citing ACC/AHA data)
The Serial Comparison Problem: When ECG #2 Contradicts ECG #1
In cardiac care, clinicians routinely compare serial ECGs to detect evolving ischemia, confirm or rule out acute coronary syndrome, and guide treatment decisions. The clinical value of this comparison depends entirely on one assumption: that both ECGs were acquired with electrodes in the same anatomical positions.
That assumption is almost never true.
In the prehospital setting, EMS personnel acquire a 12-lead ECG and typically remove the electrodes before transport or upon arrival at the emergency department. An ED nurse or technician then acquires a second ECG using their own placement. A third may follow if the patient is admitted. Each clinician identifies landmarks independently, under different conditions, with different levels of training and confidence.
Gregory et al. (2021) found that only 5.8% of paramedics placed all six precordial electrodes correctly (British Paramedic Journal). Clopton and Hyrkäs (2024) found that only 41.6% of both EMS and clinical personnel achieved acceptable placement (International Journal of Paramedicine). There is no mechanism in standard practice to ensure the second ECG replicates the first ECG’s electrode positions.
The result: two ECGs from the same patient, acquired 30 minutes apart, can show different morphologies — not because the patient’s cardiac status changed, but because the stickers moved. As a quality assessment published at one university hospital found, 50% of routine inpatient ECGs had severe artifact or were not interpretable (ScienceDirect, 2020).
CLINICAL CONSEQUENCE: When ECG #2 shows ST-segment changes that were absent on ECG #1, the clinician must decide: is this disease progression, or is this a placement artifact? In a time-critical setting, the answer to that question triggers either cath lab activation or clinical observation. One path costs tens of thousands of dollars. The other may cost a life. And neither clinician knows whether the difference is real.
The Downstream Cost Cascade: From Bad Sticker to Big Bill
The financial impact of electrode misplacement extends far beyond the cost of the ECG itself. The real damage comes from the clinical decisions that a compromised ECG triggers:
- 1. Repeat ECGs. When a tracing is artifact-ridden or shows unexpected changes, the first response is to repeat the test. Each repeat ECG costs $50–$300+ depending on the setting (hospital ED vs. clinic), consumes technician time, delays diagnosis, and may itself be compromised if the underlying placement problem persists.
- 2. Unnecessary stress testing. ECG findings suggestive of ischemia (which can be caused by electrode misplacement) frequently trigger follow-up stress tests at $200–$5,000+ per test, depending on modality.
- 3. Unnecessary cardiac catheterization. False-positive STEMI patterns from V1/V2 placed too high can trigger emergent cath lab activation at $10,000–$17,000+ per case (MedAxiom). Some studies report false activation rates of 15–40%.
- 4. Extended length of stay. Diagnostic uncertainty from inconsistent serial ECGs can extend observation periods and LOS while clinicians wait for serial troponins, additional imaging, or cardiology consultation. At an average inpatient cost of $1,170/night (MedAxiom), even one additional night per case accumulates rapidly across volumes.
- 5. Unnecessary consultations. Equivocal ECG findings often prompt cardiology consultation, consuming specialist time and adding to hospital costs.
- 6. Malpractice liability. Both missed diagnoses (false negatives from misplaced electrodes) and unnecessary procedures (false positives) represent legal exposure. Cardiovascular malpractice cases have a 75% rate of involving diagnostic error allegations and are more likely to result in death (75%) than non-cardiac malpractice cases (27%) (Quinn et al., American Journal of Medicine, 2017).
The Rehman et al. study published in Cureus quantified the downstream cost of just one consequence of lead misplacement — poor R-wave progression (PRWP). Analyzing 9,424 ECGs, they found 7.3% met criteria for PRWP, and in 10.8% of cases, precordial lead misplacement was suspected. These false patterns trigger downstream CAD assessment including stress testing and catheterization. Projected nationally, the authors estimated the cost to CMS at $3.2 billion annually — from a single artifact pattern caused by a single type of electrode misplacement.
This does not include costs from false STEMI activations, extended LOS, unnecessary consultations, or malpractice claims. The true systemic cost of electrode misplacement is almost certainly an order of magnitude larger.
Why This Keeps Happening: A Systems Failure, Not a Training Failure
Hospital administrators often assume that electrode misplacement is a training problem that can be solved with continuing education. The evidence suggests otherwise.
Clopton and Hyrkäs (2024) found that more frequent practice and classroom-based training were associated with better placement accuracy. But even among the best-performing cohorts, error rates remained clinically significant. Medani et al. (2018) demonstrated that peer-led educational interventions improved performance — yet 90% of participants still could not place all leads correctly after training.
The problem is not ignorance. The problem is that the tool itself — 10 individual adhesive electrodes applied one at a time based on manual landmark identification — is inherently variable. Different providers have different hands, different landmark identification skills, and different levels of confidence, especially with obese patients and female patients where breast tissue obscures landmarks.
Consider the operational reality:
- • ECGs in most hospitals are acquired by CNAs, ED technicians, and nurses — not dedicated ECG technicians. Few hospitals employ full-time ECG technicians.
- • Training is often informal: a printed diagram and a brief demonstration. Multiple trainees have reported being “handed a diagram and sent to acquire their first clinical ECG” (JEMS, 2025).
- • There is no standardized competency assessment or certification for ECG acquisition in the United States.
- • Electrode locations are not routinely documented on the ECG itself or in the medical record, making serial comparison unreliable by default.
- • Prehospital electrodes are routinely removed before the in-hospital ECG is acquired, ensuring that the two tracings cannot be compared from the same electrode positions.
This is not a problem you can train your way out of. It is a technology problem that requires a technology solution.
The Technology Solution: Standardizing ECG Acquisition at the Point of Care
C-Booth Innovations developed the EXG™ Wearable ECG Platform to eliminate the variability that drives serial placement inconsistency and its downstream costs. By consolidating all precordial electrode positions into a single, anatomically guided, wearable device, the EXG ensures:
- • Consistent electrode placement across every provider, every shift, every patient encounter. The anatomical guide removes individual variation from the equation.
- • Continuous monitoring from field to cath lab. Because the EXG remains in place throughout the episode of care, serial ECGs are acquired from identical electrode positions by default. No removal. No re-placement. No variation.
- • Rapid deployment under 60 seconds. Faster acquisition means less time to first ECG, meeting AHA/ACC guideline targets for 10-minute ECG acquisition.
- • Reduced repeat ECGs. Higher first-pass accuracy means fewer artifact-driven re-acquisitions, freeing technician time and improving throughput.
- • Lower total cost of ownership. Reduction in false-positive downstream testing, repeat ECGs, unnecessary cath lab activations, extended LOS, and malpractice exposure.
The EXG is FDA registered, ISO certified, designed to AHA-compliant standards, radiolucent (compatible with CT, X-ray, and interventional imaging), universally compatible with existing cardiac monitors, and expandable from 12-lead to 18-lead.
A Simple ROI Framework for Your Institution
Hospital leadership can estimate the financial impact of electrode misplacement by considering the following inputs, all of which are measurable from existing operational data:
| Cost Driver | How to Quantify |
|---|---|
| Repeat ECGs due to artifact/quality issues | Track repeat ECG rate per month × cost per ECG ($50–$300+) |
| False-positive STEMI cath lab activations | False activation rate × per-activation cost ($350–$17,000+) |
| Extended LOS from diagnostic uncertainty | Avg. additional observation hours from equivocal ECGs × hourly cost |
| Unnecessary stress testing / catheterization | Downstream testing rate on equivocal ECGs × per-test cost |
| Cardiology consultation for ECG discrepancies | Consult rate for serial ECG discrepancies × cost per consult |
| Malpractice exposure (missed MI, unnecessary procedures) | Claims history + indemnity costs (avg. ~$400K per cardiac malpractice payment) |
| Technician time on repeat acquisitions | Minutes per repeat × hourly wage × frequency |
Even a conservative estimate — reducing repeat ECG rates by 20%, false cath lab activations by 10%, and average LOS by 0.5 days for equivocal-ECG patients — represents hundreds of thousands of dollars in annual savings for a mid-sized hospital, with significant additional savings from malpractice risk reduction.
The Bottom Line for Hospital Leadership
The ECG is your most frequently performed cardiac diagnostic. It costs $16 to acquire but can trigger $10,000+ in downstream testing when acquired incorrectly. It is performed by your least-trained clinical staff using a tool that has not meaningfully changed since 1943. And when it is repeated with different electrode placement, it creates the illusion of disease progression where none exists — or hides real progression that demands immediate action.
Every serial ECG comparison in your hospital is a diagnostic gamble on whether two different people, in two different rooms, at two different times, placed 10 stickers in the same 10 places. The published evidence says they almost certainly did not.
The cost of this problem is not a line item on your P&L. It is embedded in your repeat rates, your false activation rates, your LOS, your unnecessary consultations, your downstream testing, and your malpractice reserves. It is real. It is measurable. And it is solvable.
References
- Rehman A, et al. Precordial ECG Lead Mispositioning: Its Incidence and Estimated Cost to Healthcare. Cureus. 2020;12(7):e9040.
- Gregory P, Kilner T, Lodge S, Paget S. Accuracy of ECG chest electrode placements by paramedics. British Paramedic Journal. 2021;6(1):8–14.
- Clopton E, Hyrkäs EK. Assessing the Accuracy of ECG Chest Electrode Placement by EMS and Clinical Personnel. International Journal of Paramedicine. 2024;(6):29–47.
- Medani S, et al. Accuracy in precordial ECG lead placement: improving performance through a peer-led educational intervention. Journal of Electrocardiology. 2018;51:50–54.
- GE HealthCare. The Costs of ECG Misdiagnosis Due to Poor R-Wave Progression. 2021.
- GE HealthCare. ECG Lead Misplacement: Looking at Common Issues. 2021.
- Hillrom/Baxter. Three Factors That Could Be Impacting Your ECG Interpretation. 2023. (Citing ACC/AHA data on 5% lead reversal rate.)
- Clopton E. 12-Lead ECGs: Room for Improvement. JEMS. 2025.
- ScienceDirect. Standardization in Performing and Interpreting Electrocardiograms. American Journal of Medicine. 2020.
- AHA. Automated and Interpretable Patient ECG Profiles. Circulation: Cardiovascular Quality and Outcomes. (>100M ECGs annually in U.S.)
- GE HealthCare. Retrospective Analysis of ECG Data. (300M+ ECGs worldwide annually.)
- MedAxiom. Cath Lab Profitability Analysis. (Average procedural costs, LOS costs.)
- Quinn GR, et al. Missed Diagnosis of Cardiovascular Disease in Outpatient General Medicine: Insights from Malpractice Claims Data. American Journal of Medicine. 2017.
- Hadjiantoni A, et al. Systematic review of ECG electrode placement. Cardiology and Cardiovascular Medicine. 2021.
- Walsh B. Misplacing V1 and V2 can have clinical consequences. American Journal of Emergency Medicine. 2018;36(5):865–870.
- Degheim G, et al. False activation of the cardiac catheterization laboratory. JRSM Cardiovascular Disease. 2019.
- Rao S, et al. 2025 ACC/AHA/ACEP/NAEMSP/SCAI Guideline for the Management of Patients With Acute Coronary Syndromes. Circulation. 2025.
- Naidu SS, et al. SCAI expert consensus update on best practices in the cardiac catheterization laboratory (endorsed by ACC, AHA, and HRS). 2021.
About C-Booth Innovations
C-Booth Innovations is pioneering precision in cardiac monitoring with the EXG™ Wearable ECG Platform — founded by two emergency room physicians, inspired by the clinical need to improve the standard of patient care. To schedule a demonstration and ROI assessment for your institution, visit cboothinnovations.com or call (760) 800-2109.
© 2026 C-Booth Innovations. All rights reserved. | 5835 Avenida Encinas, Suite 118, Carlsbad, CA 92008
Ready to Improve ECG Accuracy?
See how the EXG platform can standardize electrode placement across your organization.


